
This devastating disease is often referred to as the “sneak thief of sight,” since there are very few observable symptoms in its early stages. According to the National Eye Institute, about half of all people with glaucoma aren’t even aware that they have it. Often glaucoma is not detected until a significant amount of vision has been lost (typically the side—or peripheral—vision), and the disease is in its advanced stage. This vision loss cannot normally be reversed, even with treatment.
Risk Factors for Glaucoma
Anyone can develop glaucoma, but some people are at a higher risk than others. Factors that may increase your risk of developing glaucoma include:
- Being over age 60.
- Having a family history of glaucoma.
- Experiencing a serious eye injury (even if it occurred in childhood).
- Being of a particular descent, such as African-American, Latino, Caribbean or Asian.
- Having uncontrolled diabetes.
- Having uncontrolled high blood pressure or heart disease.
- Having myopia (nearsightedness).
- Using certain medications, such as corticosteroids, for prolonged periods of time.
Glaucoma and Nearsightedness
One of the factors noted above, nearsightedness has been of particular interest to researchers in recent years. Many have conducted studies showing how nearsightedness may boost a person’s risk for glaucoma. A landmark study along this line was conducted by Dr. Nomdo Jansonius at the University Medical Center Groningen in the Netherlands, and published in the journal Ophthalmology in 2011. The researchers found that, overall, nearsighted people were about 90 percent more likely to also develop “open-angle” glaucoma, the most common form of the disease, than people with normal vision.
Lifestyle Factors
In addition to the above list, certain lifestyle choices can potentially increase eye pressure, which in turn can put someone at higher risk for glaucoma. There is evidence that playing high resistance wind instruments, cigarette smoking, drinking caffeinated coffee, wearing tight neckties, being overweight or obese, alcohol consumption and illegal drug use may all increase intraocular eye pressure. Considerable research has been conducted on these topics.
In 2012, a joint study was carried out by researchers from Brigham and Women’s Hospital and Harvard Medical School which showed a possible link between heavy caffeinated coffee consumption and increased risk of developing “exfoliation glaucoma,” especially in women with a family history of glaucoma. Exfoliation glaucoma occurs when a white fibrillary material builds up on the lens of the eye and exfoliates (or rubs off) the pigments in the iris, blocking the flow of liquid out of the eyeball, leading to increased pressure and changes in the optic nerve. This study, which was published in the journal, Investigative Ophthalmology & Visual Science, found that compared to non-caffeinated coffee drinkers, people who drank three or more cups of caffeinated coffee a day were at an increased risk of developing exfoliation glaucoma. Interestingly, the researchers found no associations with the consumption of other caffeinated beverages such as cola, tea or hot chocolate, or decaffeinated coffee.
Dr. Ashraf reiterates that these findings do not mean everyone should stop drinking coffee. Instead, the take-home message is that people should drink coffee and other caffeinated beverages in moderation, especially if they have a family history of glaucoma. Regular eye exams by an ophthalmologist are also important.
Another research project related to lifestyle choices that are particularly noteworthy addressed the link between cocaine use with increased risk of glaucoma. This study was conducted by researchers at the Veterans Health Administration in Indianapolis, and published in the September 2011 issue of the Journal of Glaucoma. The researchers analyzed records for 5.3 million veterans (91 percent of whom were men) seen in Department of Veterans Affairs outpatient clinics over a one-year period and found that current and former cocaine users had a 45 percent increased risk of open-angle glaucoma. Use of amphetamines and marijuana was also significantly associated with the development of this disease, although to a lesser degree than cocaine.
How can Glaucoma be Prevented?
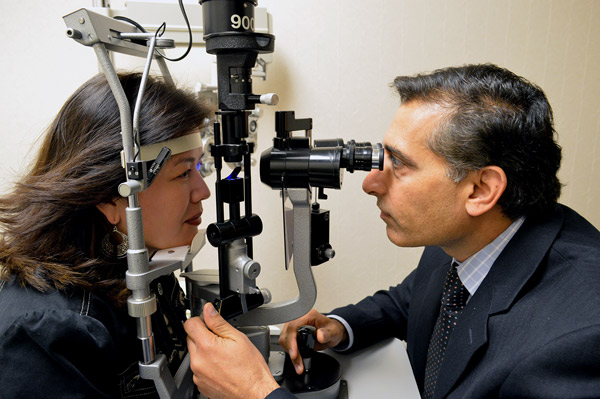
In addition to keeping up with routine eye exams, there are steps you can take to lower your risk of developing glaucoma. This includes:
- Keep your blood pressure at a normal level.
- Maintain a healthy weight.
- Don’t smoke.
- Limit your caffeine intake to moderate levels.
- Exercise at least several times a week by walking, swimming, or doing aerobics, sprint-burst type exercises or strength training.
- Eat a healthy diet. Consume abundant amounts of colorful fruit and vegetables which are rich in antioxidants, and fish or nuts high in omega-3 fatty acids. Limit your intake of highly processed, junk and high-fat foods.
- Wear eye protection while using power tools at work or playing high-speed racket sports on enclosed courts.
- When outside, prevent overexposure to sunlight by wearing sunglasses and hats.
What if worse comes to worst, and despite taking preventative measures you are diagnosed with glaucoma? In these situations, eye drops can be prescribed to help reduce the elevated intraocular eye pressure and prevent damage to the optic nerve. However, in order to be effective, these drops must be used as prescribed to prevent the progression of the disease. Surgical treatments are also available to help lower eye pressure.
The bottom line is that although glaucoma is not preventable and presently has no cure, it can be controlled if diagnosed and treated early by a licensed eye doctor.

Please Take Our LASIK or Cataract Surgery Quiz
Take our vision quiz to find out if you qualify for LASIK or cataract surgery!



